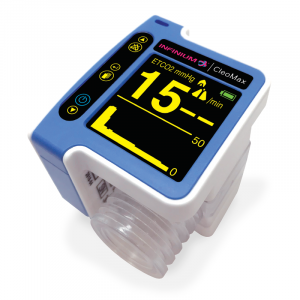
End-tidal CO2 monitoring is much more than just another number for healthcare workers to chart. End-tidal monitors have been popping up more in acute care settings, but they have actually been around for years.
Did you know that The American Society of Anesthesiologists has found that using CO2 monitoring with pulse oximetry could have prevented over 90% of anesthesia mishaps?
End-tidal CO2 monitoring is a non-invasive way to monitor a patient’s carbon dioxide levels. Both end-tidal CO2 monitors and pulse oximetry devices work closely together to help monitor the respiratory status of a patient.
So how are end-tidal CO2 monitors used? Where are they used? How do you pick the best CO2 monitoring device? Keep reading on to find the answers to these questions and to learn more about CO2 monitoring devices.
The “Ventilation Vital Sign”
In healthy individuals without preexisting lung conditions, CO2 tells a person’s body to take a breath. When CO2 levels get high, it signals to the brain to take a breath in. End-tidal CO2 monitors can give real-time breath by breath results to know what a patient’s CO2 levels are.
This is why end-tidal CO2 monitoring is sometimes referred to as the “ventilation vital sign.” Since it can tell healthcare providers how effectively the patient is breathing.
Pulse oximetry has been used for years to help healthcare providers monitor patients breathing. What is the difference between a pulse oximetry monitor and an end-tidal CO2 monitor?
Pulse oximetry monitors a patient’s blood oxygen levels. In comparison, end-tidal CO2 monitoring devices measure a patient’s CO2 levels.
Essentially, a pulse oximetry monitor is helpful in measuring the oxygen that is being delivered to someone’s body. However, end-tidal CO2 monitoring is helpful in measuring how the carbon dioxide is being used in the body.
Where CO2 Monitoring Is Used
Exhaled CO2 monitoring has been used as a standard of care in operating rooms for many years. More recently, it is being used much more in other healthcare settings inside and outside the hospital. Some areas that are starting to use end-tidal CO2 monitoring more include:
- Ambulance Services
- Emergency Departments
- Procedural Care Units
- Post-operative Units
- Intensive Care Units
These areas may use capnography for different reasons. However, they each have seen improvements in patient outcomes with ETCO2 monitoring.
Uses for CO2 Monitoring Devices
A capnograph can tell healthcare providers a lot of information about what may be going on with the patient. It may help with different diagnoses, treatments, and plans for further treatments of a patient.
End-tidal CO2 monitoring allows for almost immediate information about what is going on with a patient. This eliminates the need to wait for blood work, chest-x-rays, and other diagnostic tests.
End-tidal CO2 monitors can give healthcare providers an early warning if a patient is experiencing respiratory distress or going into respiratory failure.
Respiratory Status
CO2 monitoring can help to determine the severity of some respiratory diseases. It can also help to differentiate between some cardiac and respiratory diseases. Furthermore, it can help to determine the effectiveness of treatments.
A high CO2 level may indicate a restrictive lung disease such as COPD or asthma. When a patient is on a BiLevel PAP device or given a breathing treatment looking at their CO2 level may indicate if the treatments are helping. If CO2 levels are going down with these interventions, then these treatments are working.
However, if the patient comes into the emergency department experiencing shortness of breath, but CO2 levels are normal or low, it may mean that the patient has a cardiac-related problem such as congestive heart failure. Further testing can confirm this but, it may help guide healthcare provider’s initial treatment and testing.
An end-tidal CO2 monitor also can help monitor a patient’s respiratory status during different medical procedures.
Respiratory decline can be detected earlier during sedation procedures with end-tidal CO2 monitoring. A patient may receive too much sedative or have a lower tolerance to the sedation medication. This can cause a patient to stop breathing during the procedure or not breathe effectively.
Knowing if a patient is having changes in their respiratory status is beneficial and leads to better patient outcomes.
Endotracheal Tube Placement
End-tidal CO2 monitoring has been a gold standard in the operating room for years. This is due to the benefit CO2 monitoring has for confirming endotracheal tube placement. Capnography is the most reliable and immediate way to determine endotracheal tube placement.
Suppose a patient is in the intensive care unit, and an endotracheal tube was to become dislodged when turning the patient in the bed. With end-tidal CO2 monitoring, the healthcare professionals will be able to determine right away that the endotracheal tube dislodged and fix the situation immediately.
Cardiac Arrest
If a patient’s heart stops and a patient goes into cardiac arrest, end-tidal CO2 monitoring can help healthcare providers determine if chest compressions are being performed adequately. Capnography can also let healthcare providers know if the patient’s heart starts working again on its own.
What happens if an end-tidal CO2 monitor is showing a reading lower than 10mmHg during chest compressions? Possibly, the chest compressions are not being performed fast enough or deep enough. The person who is doing chest compressions may be getting tired and needs to switch out with someone else.
If, while doing CPR, there is a sudden spike and the CO2 levels rise up, this may indicate the patient has a return of spontaneous circulation (ROSC). In other words, the patient has a pulse back.
More Than Just a Number
Although the normal range for CO2 should be between 35-45mmHg, CO2 monitoring gives healthcare providers a lot more insight into what is going on with a patient’s condition.
A low end-tidal CO2 may indicate poor perfusion, hypovolemia, or sepsis. On the other hand, a high CO2 reading may indicate airway narrowing, airway obstruction, or respiratory distress.
It can also help the healthcare provider determine if the patient is being ventilated adequately. If a patient has a high CO2 reading on the CO2 monitoring device, then larger or more frequent breaths may help to bring the CO2 levels back down to normal. If a patient has low CO2 levels, then smaller or fewer breaths may help to raise their CO2 levels.
Healthcare providers can look at various CO2 waveforms on CO2 monitoring devices as well. The CO2 waveforms can help healthcare providers determine a possible diagnosis and come up with a treatment plan.
For example, a “shark tooth” waveform may indicate an obstructive airway disease problem such as asthma.
If the healthcare provider gives a breathing treatment, the sharp angles on the waveform may improve. This will let the healthcare provider know that the breathing treatment is working.
What to Look for When Buying CO2 Monitoring Systems
Now knowing how crucial CO2 monitoring is, you must get the best end-tidal CO2 monitoring device. There are some qualities to look for when looking around for CO2 monitoring devices, which include:
- User-Friendly
- Portability
- Versatile
- Cost-effective
Capnography devices should be easy to use. This allows all staff members to be familiar with the devices and understand how to use them.
More end-tidal CO2 monitoring devices may be used if more staff is comfortable using the capnography machines. This could lead to overall better patient outcomes.
Not all CO2 monitors can be transported with patients throughout the hospital or be used in prehospital settings. Look for a CO2 monitor that is lightweight, can easily attach to a rolling stand or IV pole, and has a reliable battery backup. This will allow for easy transport and can help with patient safety.
Moving a ventilator patient throughout the hospital can be a high-risk situation. An endotracheal tube can easily get dislodged going to cat-scan or moving rooms.
Portable capnography allows healthcare providers to detect the dislodged endotracheal tube earlier.
Patients who are not intubated will also benefit from using portable end-tidal CO2 monitoring. If their respiratory status were to decline in the hallway of the hospital, the healthcare staff would be able to notice this on the capnography. This will allow for the healthcare staff to get help fast.
A good versatile end-tidal CO2 monitor should be able to be used for both intubated and non-intubated patients. They should also have the capability to use continuous monitoring or spot checks. This will allow for capnography monitoring to be used for more patients.
Hospital equipment can be expensive, so finding good and reliable equipment for a good price is necessary. This is so your hospital can purchase enough of these devices for every patient.
Be The Best in Patient Care
CO2 monitoring is an essential tool that is being used more frequently in prehospital and hospital settings. End-tidal CO2 monitoring can help healthcare providers monitor and treat patients’ conditions better.
If you are looking for a great CO2 monitoring device that is cost-effective, user-friendly, portable, and versatile, be sure to check out Infinium Medical.
Help your hospital stand out from other hospitals by providing the best patient care with the best CO2 monitoring equipment. Contact Infinium Medical today to learn more about buying end-tidal CO2 monitors for your hospital.