As experienced clinicians and administrators, you know patient monitors are foundational to safe, efficient care across perioperative, procedural, recovery, and general medical settings. Beyond basic vital signs, today’s systems support continuous surveillance, early warning of deterioration, seamless data integration, and optimized workflows. This quick guide is a refresher for those already familiar with patient monitors, focusing on strategic selection for surgery centers and broader medical facilities. We are covering things to consider such as market options, clinical operations, and practical insights into parameters (including surgery-specific capabilities), displays, reliability, costs, connectivity, data management, and long-term ownership.
Core Functionality and Evolution
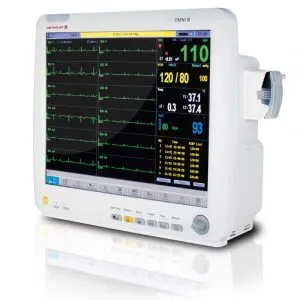
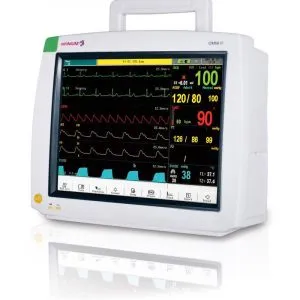
Patient monitors acquire, process, and display physiological data from sensors, generating real-time numerics, waveforms, trends, and alarms. Modern systems have evolved from standalone bedside units to networked, modular ecosystems that include portable devices, wireless telemetry, and central stations. In surgery centers, they support everything from pre-op assessment and intraoperative anesthesia to PACU recovery and step-down monitoring. Key advancements include smarter alarm algorithms to reduce fatigue, predictive analytics, and robust interoperability with hospital IT systems.
Key Measurement Parameters
Standard multiparameter monitors typically track:
- ECG (3/5/12-lead) and heart rate
- Non-invasive blood pressure (NIBP)
- Pulse oximetry (SpO2) and plethysmography
- Respiration rate
- Temperature
For surgical and procedural environments, evaluate support for advanced parameters based on your case mix:
- EtCO2/capnography and multi-gas/agent analysis — indispensable for anesthesia and sedation cases.
- Invasive blood pressure (IBP) — multiple channels for arterial, CVP, or PA lines.
- BIS or processed EEG — for depth of anesthesia and sedation monitoring.
- Cardiac output, NIBP-derived continuous BP, or advanced hemodynamics in higher-acuity procedures.
- Additional options like regional oximetry (rSO2) or neuromuscular monitoring.
Surgery-specific considerations: Anesthesia monitors in the OR often include 5-agent analysis, which simultaneously measures multiple volatile anesthetic agents (e.g., sevoflurane, isoflurane, desflurane, halothane, enflurane) along with nitrous oxide and oxygen concentrations. This capability helps confirm proper agent delivery, detect leaks or circuit issues, prevent awareness under anesthesia, and optimize emergence—critical for both safety and efficiency in mixed-procedure surgery centers.
Types of SpO2 technology: Not all pulse oximetry performs equally in challenging perioperative conditions (motion, low perfusion, vasoconstriction, or varying skin tones). Conventional 2-wavelength technology provides basic readings but can be prone to artifact. Advanced options include motion-tolerant algorithms (such as those using adaptive filtering) and multi-wavelength “rainbow” technologies that additionally measure total hemoglobin (SpHb), carboxyhemoglobin (SpCO), methemoglobin (SpMet), and pleth variability index (PVi) for fluid responsiveness assessment. When evaluating monitors for surgery and recovery, prioritize technologies validated for low-perfusion and motion-heavy environments.
Types of EtCO2 technology: Choose based on patient population and workflow. Mainstream sensors attach directly to the airway circuit for fastest response times and highest accuracy in intubated, mechanically ventilated patients—ideal for OR and deep sedation cases. Sidestream sampling aspirates gas through tubing and suits non-intubated patients or transport scenarios, though it can introduce slight delays or moisture issues. Microstream (a low-flow sidestream variant) excels with small tidal volumes, pediatric patients, or nasal cannula sampling. Many high-acuity monitors support both mainstream and sidestream modules for flexibility across procedures.
Expert tip: Prioritize modularity. Plug-in parameter modules allow scalability without replacing entire units, which is cost-effective as your procedures or patient acuity evolve. For lower-acuity areas, focus on core parameters plus strong trending and alarm customization.Types of Patient Monitors AvailableFacilities typically need a mix:
- Bedside monitors — Fixed or wall/boom-mounted for continuous OR, PACU, or room-based surveillance; often high-acuity and modular.
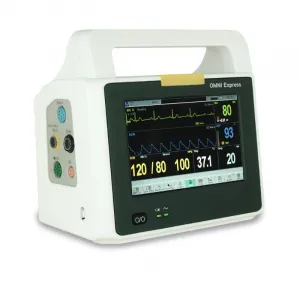
- Portable/compact monitors — Battery-powered for transport, intra-facility movement, or spot-checks; balance size with full parameter support.
- Telemetry/wireless systems — Wearable or pocket transmitters for ambulatory or step-down patients, feeding into central stations.
- Anesthesia-specific monitors — Optimized for OR integration with gas machines, 5-agent analysis, and advanced gas/EEG modules.
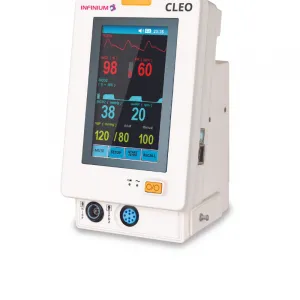
- Vital signs/spot-check monitors — Simpler, often handheld or lightweight for pre-op, triage, or outpatient areas.
- Central monitoring stations — Aggregate data from multiple bedside or telemetry units for oversight by a single team.
Consideration for surgery centers: A combination of high-acuity bedside/OR units (with robust anesthesia capabilities), portable transport monitors, and telemetry for extended recovery often provides the best coverage.
Critical Purchasing Considerations
Display Quality: Size, Resolution, and BrightnessScreen performance directly affects usability in varied lighting. Common bedside and portable sizes range from 8–15 inches; larger (12–15″) displays improve waveform visibility and multi-parameter layouts from across the room. High resolution (Full HD or better) delivers crisp traces and text, reducing interpretation errors. In ORs and brightly lit procedure rooms, prioritize high brightness (500–1000+ cd/m²) with anti-glare surfaces and wide viewing angles. Touch interfaces should support glove use and frequent disinfection.
Practical insight: Demo units under your actual lighting conditions. Customizable screen layouts and multi-monitor viewing options can enhance team coordination.
Reliability and Build Quality
Look for rugged construction that withstands frequent cleaning, transport, and 24/7 operation. High MTBF ratings, sealed ports, and proven sensor accuracy matter. Intelligent alarm systems with adjustable priorities and delay features help manage alarm fatigue—a persistent challenge in busy facilities. Cybersecurity features (e.g., encryption, role-based access, regular security updates) are now non-negotiable for connected systems.
New Versus Refurbished Monitors
New units provide the latest algorithms, software platforms, expanded connectivity, and full warranties—ideal for OR anesthesia stations or when cutting-edge features (predictive alerts, advanced integration) add clinical value.
Certified refurbished monitors offer substantial savings (often 30–60% or more) while delivering reliable performance when properly restored with OEM or equivalent parts, updated software, and warranties. They are particularly suitable for supplementary portable or telemetry units or lower-acuity areas.
Decision guidance: Assess total expected lifespan, service availability, and your risk tolerance. For mission-critical applications, lean new or top-tier refurbished from trusted sources. Always verify refurbishment processes, calibration records, and remaining economic life.
Cost and Total Cost of Ownership (TCO)
Upfront prices vary widely—basic portable or spot-check units start in the low thousands, while fully equipped high-acuity modular systems (including 5-agent and advanced SpO2/EtCO2 modules) can reach tens of thousands per unit. TCO is more important: factor in accessories/consumables, service contracts, training, software licenses, and potential downtime costs. Energy-efficient designs and modular upgrades can lower long-term expenses.
Proprietary Accessories and Ecosystem Lock-In
Many platforms rely on vendor-specific cables, sensors, modules (including agent analysis and specialized SpO2/EtCO2 sensors), and disposables, which can drive recurring costs and limit flexibility. Evaluate the total ecosystem during procurement—price and availability of replacements over 5+ years, standardization potential across units, and upgrade paths. More open or hybrid systems may reduce lock-in but require careful compatibility testing.
Expert advice: Request detailed consumables pricing and negotiate volume or multi-year accessory agreements. Standardizing on one or two platforms facility-wide simplifies training and inventory but demands strong vendor support.
Connectivity, HL7 Integration, and Data Management
Seamless integration into your hospital IT infrastructure is essential for modern workflows. Look for robust wired (Ethernet) and wireless (Wi-Fi) connectivity that maintains reliable data transmission during patient transport or across departments. HL7 (Health Level Seven) compatibility—or the newer FHIR standard—enables automatic, bidirectional data exchange with EHR/EMR systems. This supports real-time charting of vital signs, waveforms, alarms, and trends, dramatically reducing manual documentation errors, improving regulatory compliance, and freeing clinical staff for direct patient care.
Data management features should include configurable short- and long-term trending, full-disclosure waveform storage and retrospective review, event logging with searchable timestamps, and flexible export options (PDF, CSV, or direct archive integration). Centralized data aggregation—whether through on-premise servers or secure cloud solutions—facilitates quality improvement projects, morbidity/mortality reviews, research, and performance benchmarking. In surgery centers, these capabilities are particularly valuable for analyzing perioperative events, optimizing protocols, and supporting accreditation requirements.
Expert insight: Test connectivity and HL7 interfaces in your actual network environment, including bandwidth demands, firewall compatibility, failover scenarios, and multi-vendor interoperability. Prioritize monitors with strong cybersecurity (end-to-end encryption, secure boot, vulnerability management, and audit logs) to safeguard protected health information. Poor integration can create data silos or documentation burdens that negate many clinical benefits.
Making an Informed Selection
Start with a needs assessment: map your procedures, patient volumes, acuity levels, existing infrastructure, and pain points (e.g., alarm fatigue, transport delays, documentation burden, or data silos). Involve a cross-functional team—anesthesiologists, nurses, OR managers, biomedical engineering, and IT—for input. Request live demonstrations and short-term trials in your environment, specifically testing anesthesia features like 5-agent analysis, SpO2 performance during motion, EtCO2 accuracy across mainstream/sidestream setups, HL7 data flows, and network stability. Compare TCO projections, service response SLAs, and references from similar facilities. Cybersecurity reviews and regulatory compliance (FDA clearance, IEC standards) should be baseline.
Patient monitors represent a major capital and operational investment, but the right mix enhances safety, efficiency, and staff satisfaction while supporting scalable care delivery. Focus on clinical relevance—particularly perioperative anesthesia capabilities—connectivity, data management, long-term reliability, and total value rather than isolated features or lowest initial price. Thoughtful procurement today prevents costly limitations or replacements tomorrow. If your facility faces unique constraints (budget, space, network complexity, or specialized procedures), independent clinical engineering or IT consultation can provide unbiased guidance.